March 25, 2024

What is TMJ?
The temporomandibular joint (TMJ) connects the jaw to the skull on either side of the face. When it functions incorrectly, it can lead to an array of complications, including:
- Pain
- Swelling
- Face tenderness
- Clicking, popping, or grating sound when opening or closing the mouth
- In some cases, the jaw may become stuck in an opened or closed position
- Pain in the neck
- Ringing in the ears
- AND even vertigo.
TMJ is treated here at the Osteopathic Health Centre, Dubai.
What is Vertigo and How is it Connected to TMJ Condition?

Vertigo is described as a sensation that your surroundings are moving. Often, you will feel as though you are spinning, whirling, or moving in either a horizontal or vertical position. During these, there may be involuntary eye movements, hearing loss, and nausea.
Vertigo is often caused by an inner ear issue. However, a TMJ condition can also lead to what’s known at TMJ dizziness. The feeling of dizziness can often give patients a fear of falling. It may lead to a slip or fall, thereby not only resulting in injuries but also a phobia of going out in public places. It can have a big impact on day-to-day life.
The TMJ joint has a very close relation to the inner ear. The Labyrinth is found in the temporal bone at the head region of the human body. The TMJ is also attached to this temporal bone and skull. The Labyrinth plays an important role in the body’s balance and vestibular system (eyes, nerves, joints and bones). A disruption in any part of the vestibular system sends wrong signals to the brain which results in TMJ dizziness or vertigo.
How can Osteopathy help?
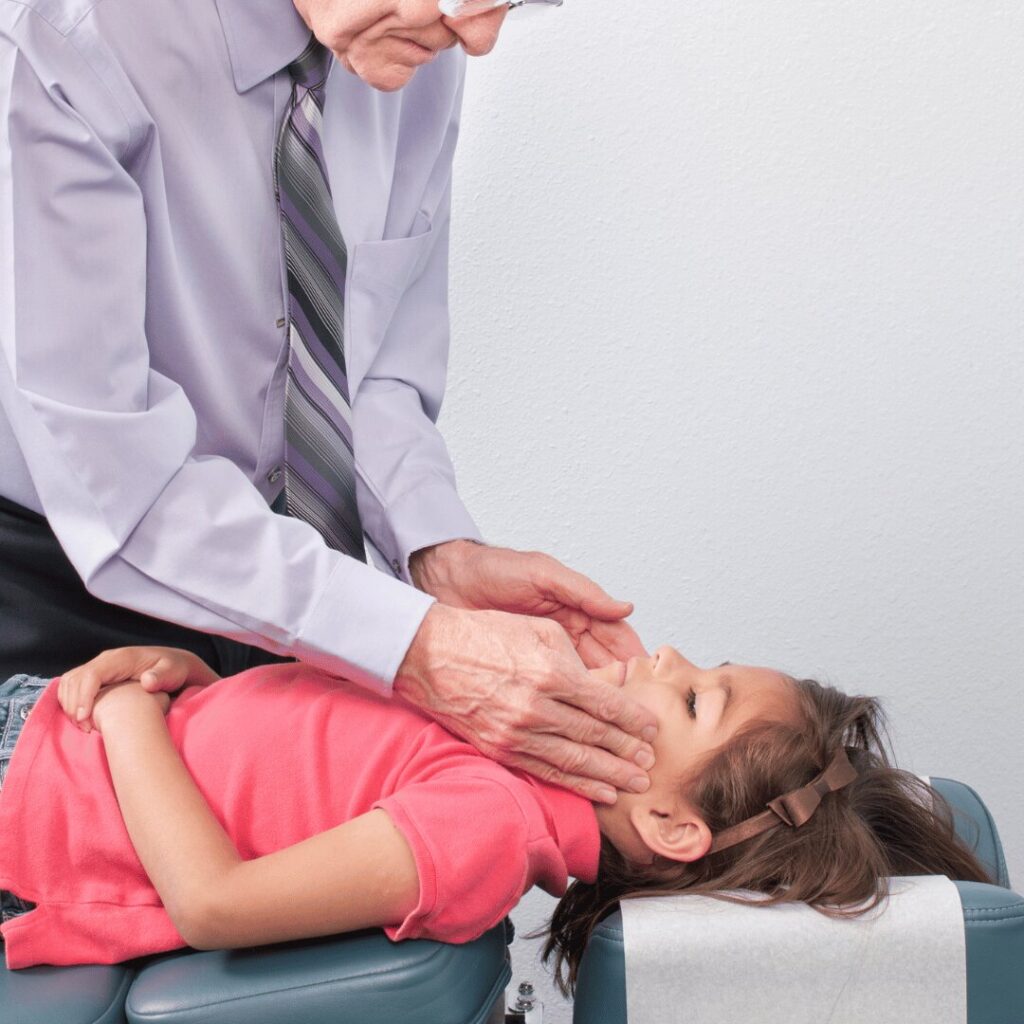
An osteopathic approach to treating TMJ dysfunction includes a thorough assessment of the head, jaw, neck, shoulders and mid-back. Due to the proximity of the jaw and neck, you rarely get dysfunction in one without the other.
Osteopaths can relieve the tightness in the soft tissue structures around the TMJ and other structures in the neck and head where the muscles of the jaw attach.
Treatment may involve:
- Soft tissue to the muscles surrounding the jaw
- Joint articulation to improve movement and biomechanics of the joint
- Dry needling to aid capsular pain and help ease arthritic pain
- Posture correction – to address any underlying biomechanics that may be contributing to jaw pain
- A combination of intra-oral and external techniques
- muscle energy techniques and isometric exercises
- Education into preventative methods such as exercises to improve posture and breathing and mindfulness advice to help manage stress
- Referral to other healthcare professionals in instances where dental care or a mouth guard are required
- Follow up exercises are prescribed to do at home for maintenance